Research News: Study Sheds Novel Insights on the Mechanism of Melanin Formation
January 10, 2023
Researchers report that a key transcription factor “Nrf3” regulates the process of melanin production in mouse and human cells
The skin serves as a physical barrier against external assaults. It also produces melanin to protect our body from DNA damage, genetic mutations, and skin cancer. Although abundantly found in the basal layer of the epidermis, the precise role of the transcription factor “Nrf3” in melanogenesis—the complex process of melanin production—remains unknown. Researchers from Doshisha University, Japan have recently unraveled Nrf3-mediated mechanism of melanogenesis, which can guide skin pigmentation-related therapeutic and pharmaceutical research.
The skin is presumably the largest and one of the most versatile body organs. By providing a physical barrier, it protects our body from environmental assaults. Melanin—a natural pigment produced by specialized skin cells called “melanocytes”—shields our body from the detrimental effects of ultraviolet (UV) radiation. UV radiation is responsible for DNA damage, genetic mutations, and can also lead to the onset of skin cancer. NF-E2-related factor 3 or “Nrf3”, a known transcription factor, or protein involved in the process of converting DNA into RNA, is abundantly found in the basal layer of the epidermis. However, its precise role in melanin production remains largely elusive.
Dr. Tsuyoshi Waku and his colleagues from the Laboratory for Genetic Code, the Faculty of Life and Medical Sciences and Graduate School of Life and Medical Sciences, Doshisha University, Japan have recently been able to discover the Nrf3-mediated mechanism of melanogenesis. Using in vitro experimentation, the research team showed that Nrf3 coordinates melanin production by regulating two key processes: macropinocytosis—engulfment and uptake of large amounts of fluids and membranes—and autophagy—recycling of old, damaged, abnormal cell components through controlled cellular breakdown. To this end, the researchers generated mouse malignant melanocyte (melanoma) B16F10 cells overexpressing Nrf3 or depleted the gene in normal human melanocyte (NHEM) cells and conducted a series of well-controlled experiments. This study was made available online on December 30, 2022 and published in volume 32 issue 1 of the journal Cell Reports on January 31, 2023.
Lead author of the study, Dr. Waku, Associate Professor at Doshisha University, muses, “This melanogenic study was started serendipitously. To investigate the effect of Nrf3 on the survival and growth of melanoma cells. We generated melanoma cells stably expressing Nrf3, and found by chance the positive effect of Nrf3 on melanogenesis.”
Co-authors, Sota Nakata, Haruka Masuda and Haruna Sumi, students of Doshisha University, discovered that Nrf3 upregulates the gene expression of core melanogenic factors, including Mitf, Tyr, Tyrp1, Pmel, and Oca2, in response to exogenous and endogenous inducers of melanin production, forskolin (Fsk), and αMSH. Moreover, they revealed that Nrf3 also induces the gene expression of Cln3, an autophagosome-related factor, for macropinocytic uptake of melanin precursors.In addition, they identified two autophagy-related genes targeted by Nrf3, i.e., Ulk2 and Gabarapl2, which contribute to the uptake of melanin precursors and the formation of melanosomes—specialized organelles responsible for the synthesis, storage, and transport of melanin.
Says co-author, Ayaka Wada, a student of Doshisha University, “We showed that Fsk or αMSH induced melanin production in B16F10 or NHEM cells in an Nrf3-dependent manner. Our immunoblotting and immunostaining results suggest that in response to Fsk, Nrf3 translocates from the ER membrane into the nucleus, where it induces melanin production and melanosome formation.” Iori Aketa, and Shuuhei Hirose, also students of the university and co-authors of the study, agree.
In fact, the researchers also found that Nrf3 triggers the recycling of skin tissues by facilitating the autolysosomal degradation of melanosomes. Furthermore, the team showed that αMSH—a hormone that stimulates melanocytes—causes Nrf3 activation and the subsequent formation of melanin, whereas nelfinavir, an HIV-1 protease inhibitor, inhibits Nrf3-mediated melanin formation.
Dr. Waku enthusiastically adds, “These findings demonstrated the physiological role of Nrf3 in the melanogenesis cascade, via the regulation of cellular membrane dynamics and the core melanogenic gene circuit, as well as the therapeutic potential of nelfinavir in skin hyperpigmentation conditions.”
The researchers are hopeful that their novel findings will be of interest not only to other scientists but also to cosmetic and pharmaceutical companies engaged in pigmentation research.
Professor Akira Kobayashi, the principal investigator of the Laboratory for Genetic Code at Doshisha University, concludes, “Our fundamental research purpose is to clarify the tumorigenic effect of Nrf3. This study implies the possibility of the pathophysiological correlation between Nrf3-mediated melanin production and melanoma malignancy.”
Melanin functions as a natural sunscreen. However, its excessive production causes melsasma, age spots, and freckles. Although further studies seem warranted, the study does seem to establish a likely association between melanin overproduction and skin cancer.
Reference
| Title of original paper | The CNC-family transcription factor Nrf3 coordinates the melanogenesis cascade through macropinocytosis and autophagy regulation |
| Journal | Cell Reports |
| DOI | 10.1016/j.celrep.2022.111906 |
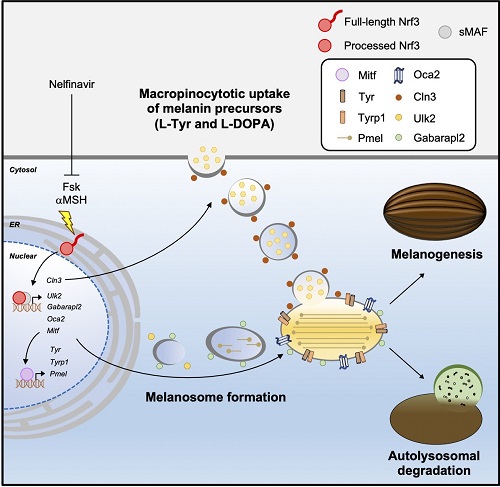
Mechanistic insights into Nrf3-mediated melanogenesis
Researchers from Doshisha University suggest that a transcription factor “Nrf3” coordinates the melanogenesis pathway in response to forskolin or αMSH via macropinocytosis and autophagy. They also indicate that nelfinavir inhibited Nrf3-mediated melanogenesis.
Image courtesy: Tsuyoshi Waku from Doshisha University
Image license: CC BY 4.0
Funding information
This study was supported in part by a grant-in-aid for Scientific Research (C) (19K07650 and 22K07219 to Tsuyoshi Waku); a grant in-aid from the Inamori Foundation (to Tsuyoshi Waku); a grant-in-aid from the Foundation for Promotion of Material Science and Technology of Japan (to Tsuyoshi Waku); grant-in-aid for Scientific Research (B) (20H03549 to Tsuyoshi Waku, 20H04135 to Akira Kobayashi); grant-in-aid for Challenging Research (Exploratory) (21K19743 to Akira Kobayashi); and grant-in-aid from the Mitsubishi Foundation (to Akira Kobayashi); grant-in-aid for JSPS Fellows (20J20194 to Shuuhei Hirose)
Profile

Dr. Tsuyoshi Waku is serving as an Associate Professor at the Faculty of Life and Medical Sciences and Graduate School of Life and Medical Sciences, Doshisha University, Japan. He obtained his Ph.D. from Osaka University, Japan. Dr. Waku’s research group primarily conducts research in the field of gene expression, cancer development, transcription, translation, protein degradation, fat metabolism, cancer microenvironment, and tumor immunity. Dr. Waku has more than 35 publications to his credit. His work has been published in reputable journals such as Cell Reports,iScience, and Molecular and Cellular Biology.
Tsuyoshi Waku
Associate Professor , Faculty of Life and Medical Sciences Department of Medical Life Systems
Media contact
Organization for Research Initiatives & Development
Doshisha University
Kyotanabe, Kyoto 610-0394, JAPAN
CONTACT US
